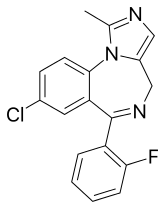
Midazolam hydrochloride

Midazolam, marketed under the trade name Versed, among others, is a medication used for anesthesia, procedural sedation, trouble sleeping, and severe agitation. It works by inducing sleepiness, decreasing anxiety, and causing a loss of ability to create new memories. It is also useful for the treatment of seizures. Midazolam can be given by mouth, intravenously, or injection into a muscle, by spraying into the nose, or through the cheek. When given intravenously, it typically begins working within five minutes; when injected into a muscle, it can take fifteen minutes to begin working. Effects last for between one and six hours. Midazolam, marketed under the trade name Versed, among others, is a medication used for anesthesia, procedural sedation, trouble sleeping, and severe agitation. It works by inducing sleepiness, decreasing anxiety, and causing a loss of ability to create new memories. It is also useful for the treatment of seizures. Midazolam can be given by mouth, intravenously, or injection into a muscle, by spraying into the nose, or through the cheek. When given intravenously, it typically begins working within five minutes; when injected into a muscle, it can take fifteen minutes to begin working. Effects last for between one and six hours. Side effects can include a decrease in efforts to breathe, low blood pressure, and sleepiness. Tolerance to its effects and withdrawal syndrome may occur following long-term use. Paradoxical effects, such as increased activity, can occur especially in children and older people. There is evidence of risk when used during pregnancy but no evidence of harm with a single dose during breastfeeding. It belongs to the benzodiazepine class of drugs and works by increasing the activity of the GABA neurotransmitter in the brain. Midazolam was patented in 1974 and came into medical use in 1982. It is on the World Health Organization's List of Essential Medicines, the most effective and safe medicines needed in a health system. Midazolam is available as a generic medication and is not very expensive. The wholesale cost in the developing world of a vial is about US$0.35. In many countries, it is a controlled substance. Midazolam is sometimes used for the acute management of seizures. Long-term use for the management of epilepsy is not recommended due to the significant risk of tolerance (which renders midazolam and other benzodiazepines ineffective) and the significant side effect of sedation. A benefit of midazolam is that in children it can be given in the cheek or in the nose for acute seizures, including status epilepticus. Midazolam is effective for status epilepticus that has not improved following other treatments or when intravenous access cannot be obtained, and has advantages of being water-soluble, having a rapid onset of action and not causing metabolic acidosis from the propylene glycol vehicle, which occurs with other benzodiazepines. Drawbacks include a high degree of breakthrough seizures—due to the short half-life of midazolam—in over 50% of people treated, as well as treatment failure in 14–18% of people with refractory status epilepticus. Tolerance develops rapidly to the anticonvulsant effect, and the dose may need to be increased by several times to maintain anticonvulsant therapeutic effects. With prolonged use, tolerance and tachyphylaxis can occur and the elimination half-life may increase, up to days. There is evidence buccal and intranasal midazolam is easier to administer and more effective than rectally administered diazepam in the emergency control of seizures. Intravenous midazolam is indicated for procedural sedation (often in combination with an opioid, such as fentanyl), for preoperative sedation, for the induction of general anesthesia, and for sedation of people who are ventilated in critical care units. Midazolam is superior to diazepam in impairing memory of endoscopy procedures, but propofol has a quicker recovery time and a better memory-impairing effect. It is the most popular benzodiazepine in the intensive care unit (ICU) because of its short elimination half-life, combined with its water solubility and its suitability for continuous infusion. However, for long-term sedation, lorazepam is preferred due to its long duration of action, and propofol has advantages over midazolam when used in the ICU for sedation, such as shorter weaning time and earlier tracheal extubation. Midazolam is sometimes used in neonatal intensive care units. When used, additional caution is required in newborns; midazolam should not be used for longer than 72 hours due to risks of tachyphylaxis, and the possibility of development of a benzodiazepine withdrawal syndrome, as well as neurological complications. Bolus injections should be avoided due to the increased risk of cardiovascular depression, as well as neurological complications.Midazolam is also sometimes used in newborns who are receiving mechanical ventilation, although morphine is preferred, owing to its better safety profile for this indication. Midazolam, in combination with an antipsychotic drug, is indicated for the acute management of schizophrenia when it is associated with aggressive or out-of-control behaviour. In the final stages of end-of-life care, midazolam is routinely used at low doses via subcutaneous injection to help with agitation, myoclonus, restlessness or anxiety in the last hours or days of life. At higher doses during the last weeks of life, midazolam is considered a first line agent in palliative continuous deep sedation therapy when it is necessary to alleviate intolerable suffering not responsive to other treatments, but the need for this is rare. Benzodiazepines require special precaution if used in the elderly, during pregnancy, in children, in alcohol- or other drug-dependent individuals or those with comorbid psychiatric disorders. Additional caution is required in critically ill patients, as accumulation of midazolam and its active metabolites may occur. Kidney or liver impairments may slow down the elimination of midazolam leading to prolonged and enhanced effects. Contraindications include hypersensitivity, acute narrow-angle glaucoma, shock, hypotension, or head injury. Most are relative contraindications.