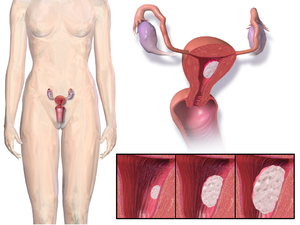
Endometrial cancer

Endometrial cancer is a cancer that arises from the endometrium (the lining of the uterus or womb). It is the result of the abnormal growth of cells that have the ability to invade or spread to other parts of the body. The first sign is most often vaginal bleeding not associated with a menstrual period. Other symptoms include pain with urination, pain during sexual intercourse, or pelvic pain. Endometrial cancer occurs most commonly after menopause. Approximately 40% of cases are related to obesity. Endometrial cancer is also associated with excessive estrogen exposure, high blood pressure and diabetes. Whereas taking estrogen alone increases the risk of endometrial cancer, taking both estrogen and a progestogen in combination, as in most birth control pills, decreases the risk. Between two and five percent of cases are related to genes inherited from the parents. Endometrial cancer is sometimes loosely referred to as 'uterine cancer', although it is distinct from other forms of uterine cancer such as cervical cancer, uterine sarcoma, and trophoblastic disease. The most frequent type of endometrial cancer is endometrioid carcinoma, which accounts for more than 80% of cases. Endometrial cancer is commonly diagnosed by endometrial biopsy or by taking samples during a procedure known as dilation and curettage. A pap smear is not typically sufficient to show endometrial cancer. Regular screening in those at normal risk is not called for. The leading treatment option for endometrial cancer is abdominal hysterectomy (the total removal by surgery of the uterus), together with removal of the fallopian tubes and ovaries on both sides, called a bilateral salpingo-oophorectomy. In more advanced cases, radiation therapy, chemotherapy or hormone therapy may also be recommended. If the disease is diagnosed at an early stage, the outcome is favorable, and the overall five-year survival rate in the United States is greater than 80%. In 2012, endometrial cancers newly occurred in 320,000 women and caused 76,000 deaths. This makes it the third most common cause of death in cancers which only affect women, behind ovarian and cervical cancer. It is more common in the developed world and is the most common cancer of the female reproductive tract in developed countries. Rates of endometrial cancer have risen in a number of countries between the 1980s and 2010. This is believed to be due to the increasing number of elderly people and increasing rates of obesity. Vaginal bleeding or spotting in women after menopause occurs in 90% of endometrial cancer. Bleeding is especially common with adenocarcinoma, occurring in two-thirds of all cases. Abnormal menstrual cycles or extremely long, heavy, or frequent episodes of bleeding in women before menopause may also be a sign of endometrial cancer. Symptoms other than bleeding are not common. Other symptoms include thin white or clear vaginal discharge in postmenopausal women. More advanced disease shows more obvious symptoms or signs that can be detected on a physical examination. The uterus may become enlarged or the cancer may spread, causing lower abdominal pain or pelvic cramping. Painful sexual intercourse or painful or difficult urination are less common signs of endometrial cancer. The uterus may also fill with pus (pyometrea). Of women with these less common symptoms (vaginal discharge, pelvic pain, and pus), 10–15% have cancer. Risk factors for endometrial cancer include obesity, diabetes mellitus, breast cancer, use of tamoxifen, never having had a child, late menopause, high levels of estrogen, and increasing age. Immigration studies (migration studies), which examine the change in cancer risk in populations moving between countries with different rates of cancer, show that there is some environmental component to endometrial cancer. These environmental risk factors are not well characterized. Most of the risk factors for endometrial cancer involve high levels of estrogens. An estimated 40% of cases are thought to be related to obesity. In obesity, the excess of adipose tissue increases conversion of androstenedione into estrone, an estrogen. Higher levels of estrone in the blood causes less or no ovulation and exposes the endometrium to continuously high levels of estrogens. Obesity also causes less estrogen to be removed from the blood. Polycystic ovary syndrome (PCOS), which also causes irregular or no ovulation, is associated with higher rates of endometrial cancer for the same reasons as obesity. Specifically, obesity, type II diabetes, and insulin resistance are risk factors for Type I endometrial cancer. Obesity increases the risk for endometrial cancer by 300–400%.